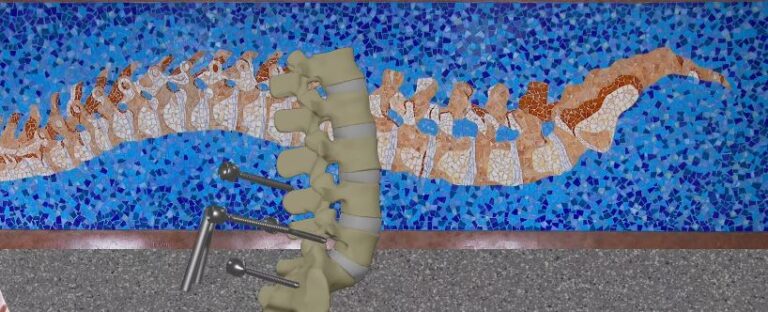
Although surgery is frequently viewed as a single step toward recovery, for some people it causes an unanticipated chain reaction. A scenario where a single procedure causes biomechanical changes, organ stress, or unanticipated complications that necessitate additional interventions is referred to as “domino effect surgery.” This cycle is still a major concern in many specialties, from organ transplantation to spinal fusion, even as modern medicine continues to improve its methods.
Spinal fusion surgery is one of the most well-known instances of the domino effect. The fusion process accelerates the degeneration of two vertebrae by shifting mechanical stress to adjacent levels. Chronic pain from this extra strain frequently necessitates yet another operation to treat the newly injured area. Patients may eventually become trapped in a cycle of repeated procedures with diminishing returns as a result of this pattern.
The Domino Effect in Surgery
| Type of Surgery | Common Domino Effect | Impact |
|---|---|---|
| Spinal Fusion | Adjacent segment degeneration | Leads to further spine surgeries |
| Organ Transplantation | Need for secondary transplants | Increases transplant waiting lists |
| Joint Replacement | Wear and tear on surrounding joints | Requires revision surgeries |
| Heart Surgery | Increased risk of secondary heart conditions | May lead to additional procedures |
| Cosmetic Surgery | Overcorrection or tissue scarring | Triggers further corrective procedures |
Another manifestation of the domino effect is seen in organ transplants, especially in domino transplants. In these operations, a patient in need of a new organ gives their own organ to a recipient who is not completely healthy but is partially functional. Although this approach broadens the pool of potential donors, it also raises the possibility of future transplants. Second-hand organ recipients frequently have shorter organ lifespans, increasing the likelihood of undergoing another surgery in the coming years.
The path of joint replacement surgery is similar. Although a patient undergoing a hip or knee replacement may initially have more mobility, the changed biomechanics may put more strain on the nearby muscles and joints. Degenerative changes brought on by this extra burden frequently call for additional surgical procedures. Younger patients are especially at risk because they are more likely to outlive their implant’s lifespan.
The ripple effect is not limited to transplant and orthopedic cases. For instance, complications from heart surgeries may necessitate further care. Changes in blood flow dynamics may occur in a patient having valve replacement, putting additional strain on the cardiovascular system. Even if the initial surgery is successful, this may eventually necessitate additional corrective procedures.
The domino effect can occur even during cosmetic procedures. A patient who has a rhinoplasty to achieve a more refined nasal shape may later have trouble breathing because of changes to their airway structures. In these situations, a revision procedure is required for functional restoration rather than aesthetic purposes. Regrettably, frequent changes raise the possibility of scar tissue accumulation, making subsequent corrections even more challenging.
Breaking this cycle is a growing focus for medical professionals. Researchers want to lower the long-term risks connected to specific procedures by developing less invasive methods. For example, artificial disc replacement has become a viable alternative to fusion in spinal surgery, allowing for more natural movement while lessening the strain on neighboring levels. The development of lab-grown organs may eventually remove the need for secondary transplants in organ transplantation, improving patient outcomes.
Patient education is the first step in preventing the domino effect. Many people have surgeries without fully comprehending the possible long-term effects. Medical practitioners can assist patients in making better decisions by giving them a more comprehensive understanding of the risks and, when practical, non-surgical alternatives. In certain situations, advanced rehabilitation programs, physical therapy, or regenerative medicine may provide just as good results without the dangers of repeated surgeries.
Notable strides are being made by certain surgical specialties in reducing the cascade of events. Improvements in prosthetic materials have greatly increased the durability of joint replacement procedures, which has decreased the need for revision surgeries. The likelihood of follow-up transplants has decreased as a result of improved immunosuppressive therapies in organ transplantation, which have increased the viability of donor organs. These advancements in medicine portend a change to longer-term care that is more sustainable.
The ethical and financial ramifications of repeated surgeries are receiving more attention than just patient outcomes. Opponents contend that the healthcare system’s financial structure favors surgeries over non-invasive therapies. High-revenue procedures are advantageous to hospitals and surgical centers, but they can occasionally result in an excessive reliance on operations that could be prevented with alternative therapies or preventive care. Systemic change is needed to address this problem, including updated treatment protocols and a focus on long-term patient health rather than temporary procedural fixes.
Surgical care is moving toward a more patient-centered future in spite of these obstacles. Physicians are attempting to reduce the need for repeated procedures by combining regenerative therapies, precision surgical methods, and personalized medicine. In order to create a more sustainable path for surgical intervention, the emphasis is now on maintaining natural function rather than treating symptoms.